2010 study
Rodrigo Noseda,1 Vanessa Kainz,1 Moshe Jakubowski,1Joshua J. Gooley,2 Clifford B. Saper,2,3Kathleen Digre,4 and Rami Burstein1,3
1Department of Anesthesia, Harvard Medical School, Boston, Massachusetts, USA
2Department of Neurology, Harvard Medical School, Boston, Massachusetts, USA
3Beth Israel Deaconess Medical Center and Program in Neuroscience, Harvard Medical School, Boston, Massachusetts, USA
4Department of Neurology and Ophthalmology, Moran Eye Center, University of Utah, Salt Lake City, Utah
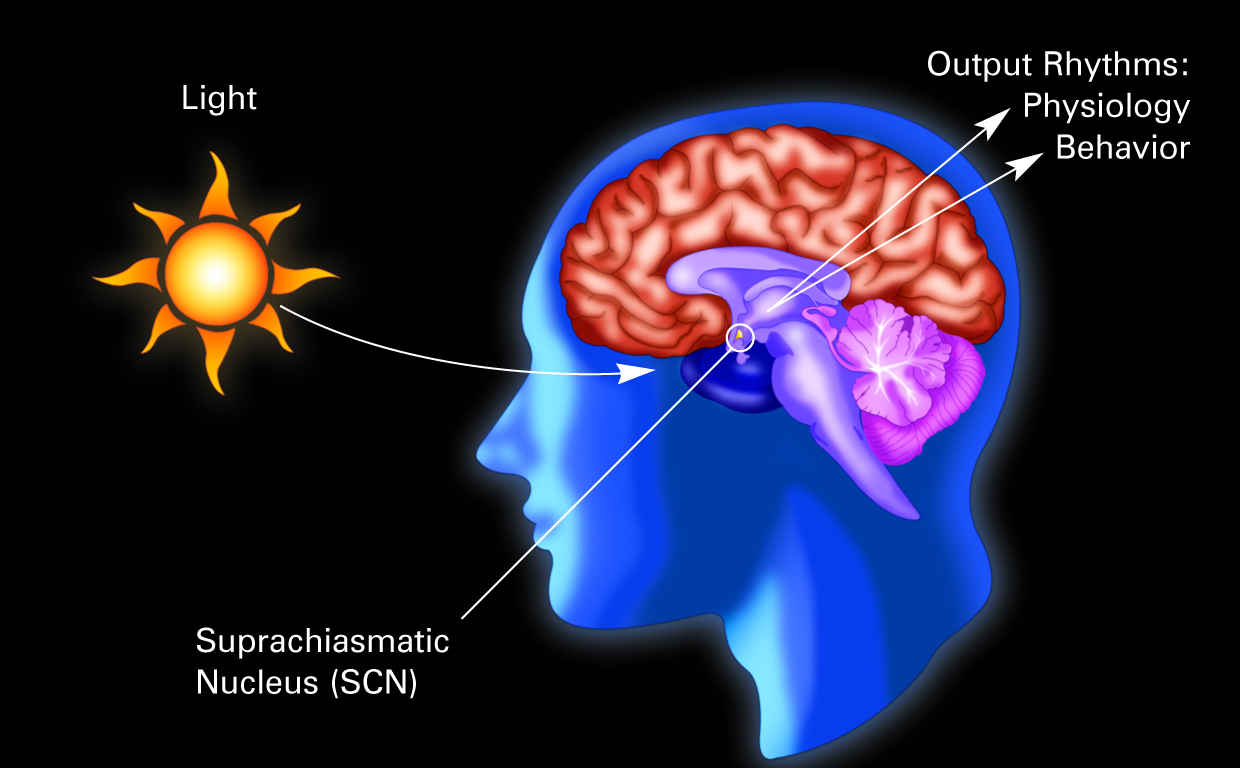
The perception of migraine headache, which is mediated by nociceptive signals transmitted from the cranial dura mater to the brain, is uniquely exacerbated by exposure to light. Here we show that exacerbation of migraine headache by light is prevalent among blind persons who maintain non-image-forming photoregulation in the face of massive rod/cone degeneration. Using single-unit recording and neural tract-tracing in the rat, we identified dura-sensitive neurons in the posterior thalamus, whose activity was distinctly modulated by light, and whose axons projected extensively across layers I through V of somatosensory, visual and associative cortices. The cell bodies and dendrites of such dura/light-sensitive neurons were apposed by axons originating from retinal ganglion cells, predominantly from intrinsically-photosensitive retinal ganglion cells – the principle conduit of non-image-forming photoregulation. We propose that photoregulation of migraine headache is exerted by a non-image-forming retinal pathway that modulates the activity of dura-sensitive thalamocortical neurons.
Whole study on this link.